If you shake the salt shaker as vigorously as I do, you probably get weird looks in restaurants. That’s because the US government recommends limiting sodium (a component of salt) to 2.3 grams per day. All in the name of heart health.
This recommendation is largely based on observational data[*][*][*] that reports higher sodium intakes are linked to higher blood pressure (hypertension) in certain populations. High blood pressure, you’re probably aware, has been an established heart disease risk factor for decades.
Other studies, however, paint a different picture about sodium. In this picture, higher salt intakes are linked to less hypertension and a lower risk of death from stroke or heart attack.
The anti-salt camp hold up their data. The pro-salt people hold up theirs. And the argument goes nowhere.
So is salt good or bad for you? I won’t lie, I have a horse in this race. I don’t think sodium is some kind of panacea or that more is always better, but based on the latest nutritional science I think it’s clear the USDA recommendation is absurdly low. Two grams of this electrolyte each day just isn’t optimal.
My belief is based somewhat on personal experience, but mostly on my analysis of the data. That’s where my biochemistry background came in handy. I went deep on this stuff. In fact, I’ve spent so much time with the sodium literature lately that I haven’t seen my family for months. (Sorry kids!)
Just kidding. I wouldn’t do that, even for sodium. But understand: This topic is super important to me and that’s why I wrote this post.
Today I’ll present both sides of the argument: pro-salt and anti-salt. Then you can decide which side makes more sense. This is called thinking for yourself. I highly recommend it!
What Sodium Does
First of all, let’s get something straight: Sodium is not an optional mineral. Even low-salt advocates (at least the ones with functioning frontal lobes) aren’t calling for zero sodium. At a bare minimum, everyone needs around 500 mg daily to squeak by—though this says nothing about optimal intakes.
If your diet is very low on salt, your body goes into sodium-sparing mode. Certain hormones kick up, and you pee out less sodium. High salt diets have the opposite effect. More on this later.
The main functions of sodium in your body include:
- Regulating fluid balance outside your cells (i.e. helping your blood flow)
- Conducting nerve impulses in your brain and nervous system
- Maintaining blood pressure
- Helping transport nutrients through your gut
Now that you know what sodium does, let’s look at how the low-salt movement began.
The History of Low-Sodium Recommendations
Lewis Dahl was a research scientist who published a number of papers in the 1960s and 1970s. Back then, he discovered that rats with certain genes—now called “Dahl rats”—would develop high blood pressure at high salt intakes.
Dahl also found a link between sodium and hypertension in human populations. The data was observational, however, and Dahl puzzled over the fact that many individuals on high salt diets did not have high blood pressure.
Dahl’s findings were used, in part, to justify 1980 US Dietary Guidelines that admonished the public to “avoid too much sodium.” These guidelines, however, didn’t say how much salt one should avoid.
This has changed. Today the USDA recommends capping sodium at 2.3 grams per day to reduce the risk of hypertension and heart disease. The American Heart Association (AHA) is even more bearish on salt, advising you to stay under 1.5 grams per day. For reference, the average American consumes about 3.4 grams of sodium per day.
Next is the fun part where we dive into the evidence. Read on.
Sodium and Blood Pressure
A number of studies (mostly observational, though some clinical) point to salt’s role in increasing blood pressure. Physiologically, this isn’t surprising. If I inject you with loads of sodium, it will increase your blood volume, and therefore your blood pressure.
But what about normal variations in dietary sodium intake? How does that affect blood pressure?
The data aren’t consistent. Take the Intersalt Study, published in 1988, which looked at sodium and blood pressure in over ten thousand people across 52 regions of the world. In the vast majority of populations, researchers observed no link between sodium intake and high blood pressure. But some outlier populations stood out.
For instance, the Yanomamo (native to Brazil) ate very little sodium and had—much to the glee of anti-salt folks—very low blood pressure. To them, this correlation was data to vindicate low-salt diets. But the Yanomamo aren’t exactly ideal models for the low-salt campaign. In fact, this population die relatively young and appear to suffer from growth issues. This isn’t to say that inadequate sodium is the cause of their health woes, but it’s not exactly protecting them from the outcomes that matter most.
Since the Intersalt Study, evidence for sodium causing high blood pressure continues to underwhelm. In 2017, researchers analyzed 2,632 people with normal blood pressure consuming either low (under 2.5 grams) or high (over 2.5 grams) sodium intakes. Guess what? The high sodium group had lower blood pressure than the salt restrictors. This simply couldn’t happen if more sodium always meant higher blood pressure.
The Potassium Connection
A subset of the population are genetically prone to hypertension at high salt intakes. We call these people “sodium hyper responders,” and their data is intermingled with everyone else’s—likely driving many positive correlations between sodium intake and blood pressure.
Should salt-sensitive people avoid salt then? Not necessarily. They may do better to increase potassium—another crucial electrolyte abundant in fruits and vegetables.
When salt-sensitive people eat enough potassium (3.5–5 grams per day is a good evidence-based target), it neutralizes the effect of sodium on blood pressure. This effect also occurs, to a lesser extent, in the rest of the population.
Inadequate potassium could explain some data linking high sodium diets to hypertension. High sodium diets tend to be full of refined foods, which are notoriously devoid of potassium.
People eating more sodium also tend to consume more soft drinks. We know soft drinks cause obesity, and obesity drives hypertension. Maybe it’s soft drinks, not sodium, driving this connection. The point is that food quality matters tremendously. Something to chew on.
Does Low Sodium Help Your Heart?
The case for sodium restriction lowering blood pressure is tenuous at best. But even if we buy that argument for a moment, what about the outcomes that really matter? Do low-sodium diets actually prevent heart attacks, strokes, and cardiac death?
In my opinion, the best answer to this question was published in the Journal of the American Medical Association (JAMA) eight years ago. Researchers followed 4,729 heart disease patients over several years, routinely measuring sodium excretion as a proxy for sodium intake. When the study wrapped, 2,057 of the patients had died from stroke, heart attack, and other cardiac-related deaths. Researchers then plotted the risk of death data against the sodium intake data:
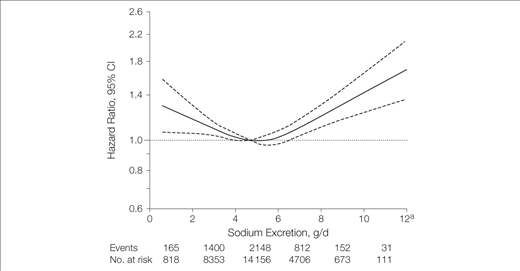
As you can see, the lowest risk of death (bottom of the U) aligns with about 4–6 grams of sodium per day. Travel left from this spot to lower sodium intakes and the death risk shoots up.
More recently, researchers reviewed a bunch of clinical trials on low-sodium diets for treating heart failure. They found no good evidence to support low-sodium diets.
At least according to this data, low-sodium diets don’t improve heart health. But there’s still massive confusion on this point. You can thank sprawling organizations like the USDA and AHA for that.
It’s worse than harmless confusion though. Hiding the salt shaker may actually be doing harm.
The Dark Side of Low Sodium Diets
When you restrict salt, your kidneys go into sodium-sparing mode. In other words, you pee out less sodium.
Think of it like wartime rations. When sodium is scarce, you save some for later. Your body is smart like that.
Preserving sodium, however, comes with consequences. Namely, a flood of hormones like aldosterone, renin, and norepinephrine with potentially undesirable effects.
Both renin and aldosterone, for instance, raise blood pressure. And norepinephrine isn’t a “bad” hormone per se. It helps get you going. But norepinephrine is also part of the stress response, and boosts levels of the blood-pressure-spiking renin.
But the biggest danger of low sodium diets? They increase the risk of hyponatremia (low blood serum sodium) and the muscle cramps, fatigue, seizures, confusion, and brain damage that often come along with it.
By itself, a low sodium diet probably won’t cause hyponatremia. The main causes are heart failure, kidney disease, liver disease, cancer, diuretic usage, vomiting, diarrhea, and (the one that really irks me) overhydration with plain water.
But getting enough sodium gives you a baseline of protection, especially against the exercise-associated form of hyponatremia. A few populations in particular must work extra hard to get enough sodium and avoid this condition:
- Athletes, who lose lots of sodium through sweat. The Journal of Sports Science estimates that athletes have daily sodium losses of 3.5-7 grams. Note: this is in addition to their baseline sodium need.
- Low-carb or keto dieters, who excrete extra sodium thanks to low insulin levels.
- Those who practice fasting, who lose lots of sodium due to the natriuresis of fasting.
I fall into all three of these categories, and for years I struggled on and off the jiu-jitsu mat to maintain my energy. Finally, with the help of my former coaches, I realized I wasn’t getting enough sodium. When I started taking a daily electrolyte powder, I felt like I’d jumped on a mushroom in Super Mario. (Not a drug reference, folks!)
I’m not saying my story applies to everyone. But when you look at the data on sodium, it seems to me that people need more—not less—of this electrolyte.
The government says stay under 2.3 grams, the average American eats about 3.4 grams, and the sweet spot for heart outcomes is closer to 4–6 grams. I shoot for that last target.
For more on my sodium (and other electrolyte) protocols, check out a couple of our other articles:
Thanks for reading!

